
Peptide Therapy in New York City
Precision at the
Molecular Level
Where biochemistry meets the art of the smile. At Core Smiles, we integrate evidence-based peptide protocols alongside your dental care — working at the biological level to heal, strengthen, and protect.
The Science of Peptides
Small Molecules.
Profound Results.
Peptides are short chains of amino acids — the fundamental language your body uses to signal cellular behavior. Unlike broad-spectrum treatments, targeted therapeutic peptides communicate directly with specific tissues: enamel matrix proteins, collagen-producing fibroblasts, muscle spindles, and immune mediators.
At Core Smiles, we sit at the intersection of advanced dental medicine and systemic wellness. Our approach integrates peptide protocols alongside traditional care to address the root biology of the conditions we treat — from enamel erosion and periodontal breakdown to TMJ myofascial pain and chronic oral inflammation.
This is dentistry practiced at its highest level — not just restoring what has been lost, but optimizing the biological environment for lasting health.

Therapeutic Peptide Directory
Peptides That Serve
the Oral System
Each peptide category below is supported by clinical research and available today through compounding pharmacies or commercially manufactured formulations.
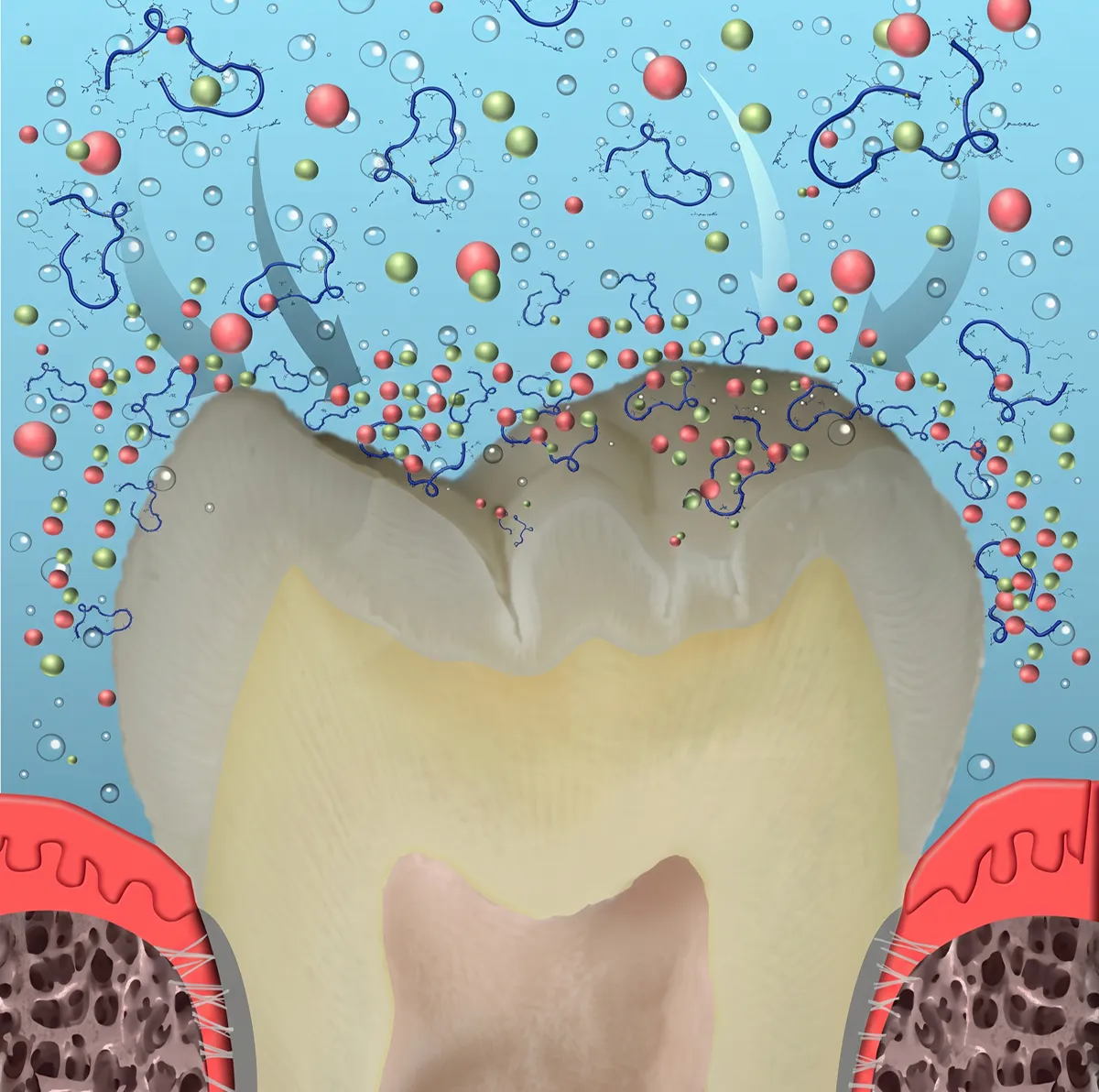
Enamel Regeneration
Amelogenin-Derived Peptides
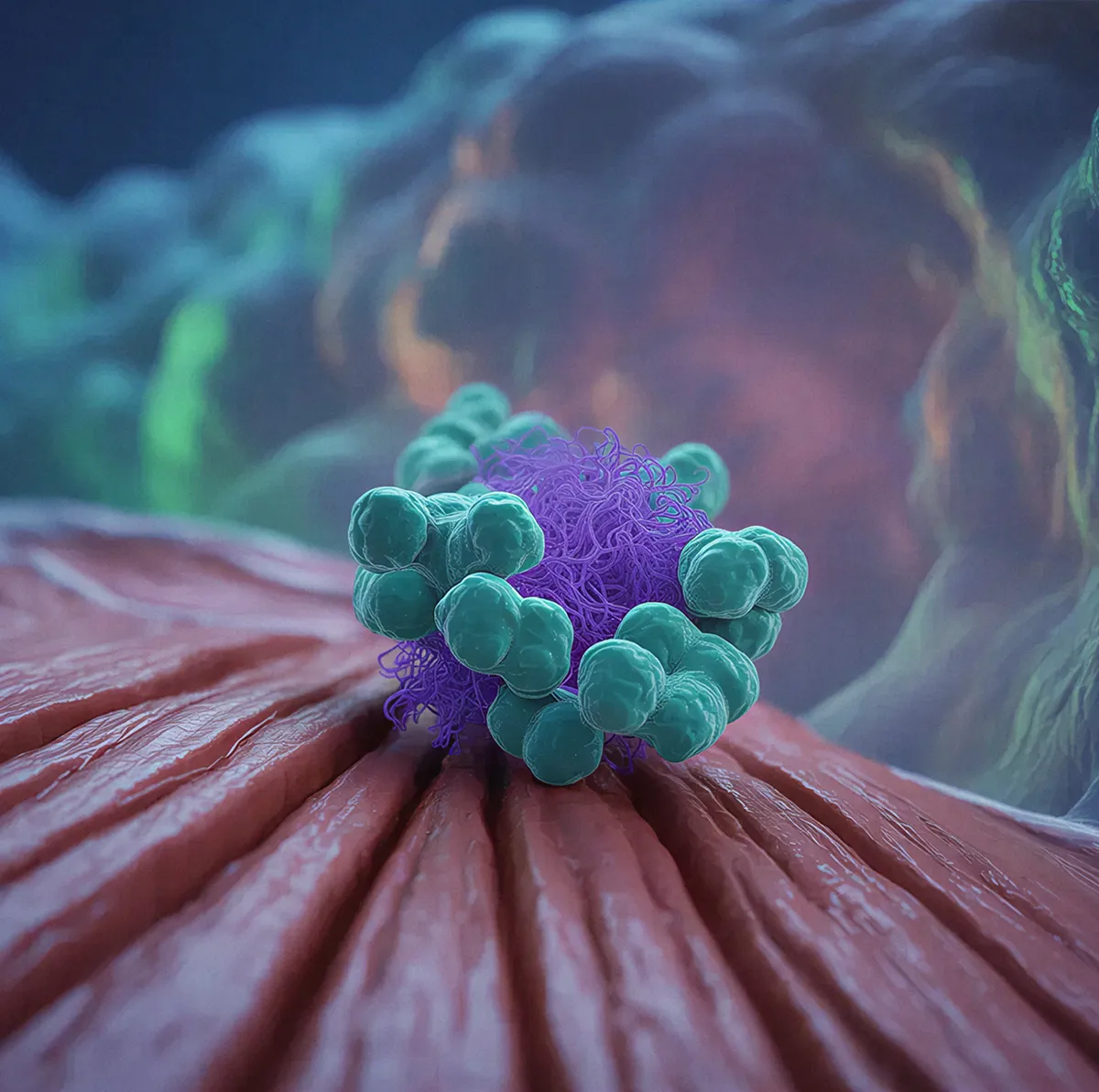
Muscle Repair & TMJ
BPC-157

Collagen & Periodontal
GHK-Cu

Anti-Inflammation
Thymosin Beta-4
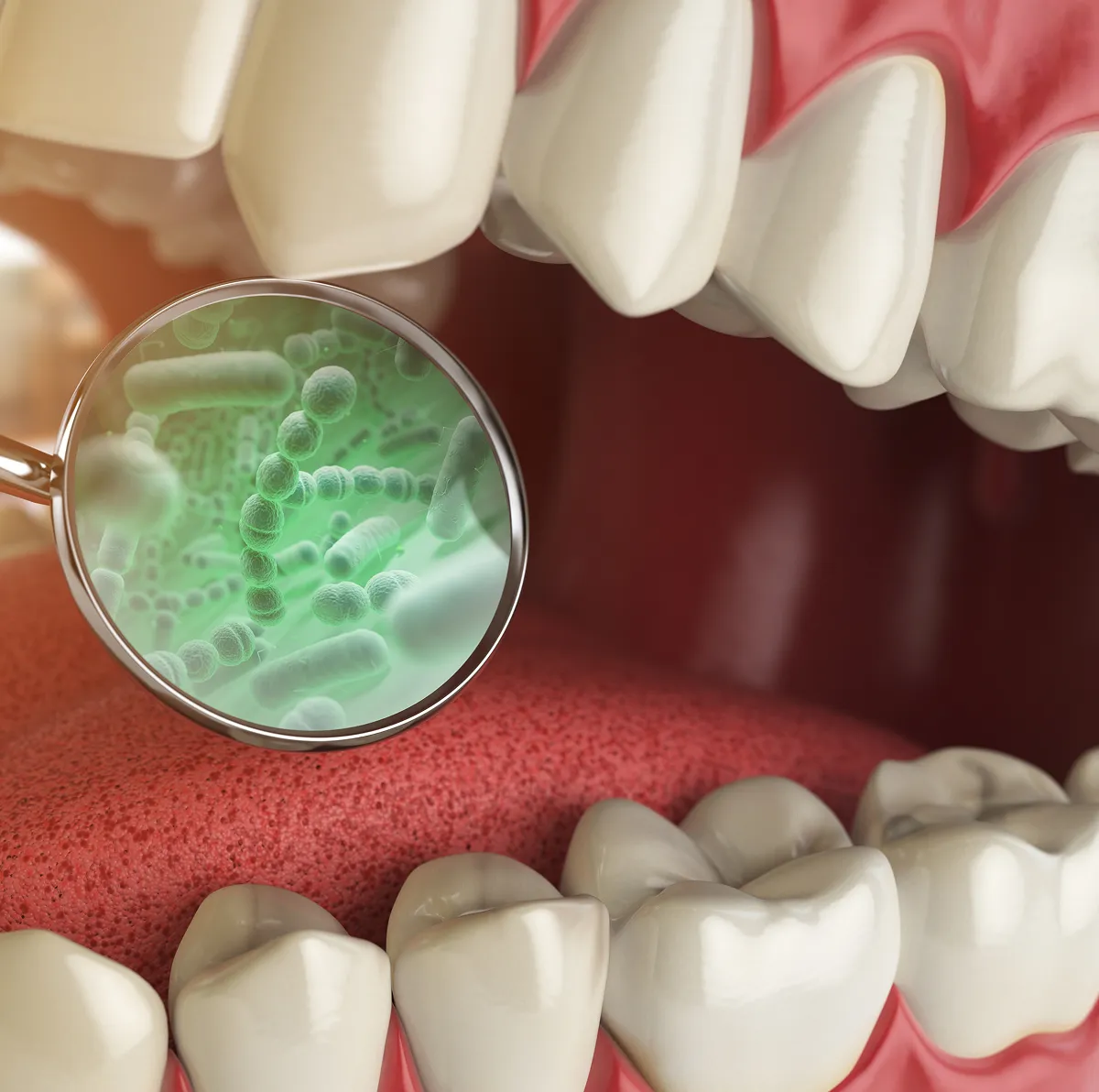
Systemic Anti-Inflammatory
KPV & Larazotide
Bone & Tissue Growth
CJC-1295 / Ipamorelin

Sleep & Bruxism
Selank & DSIP

Oral Microbiome
Antimicrobial Peptides
BPC-157 Deep Dive
How Peptides Work
in the Oral System
01
What is it?
Body Protection Compound-157
BPC-157 is a synthetic 15-amino acid peptide derived from a naturally occurring protein in human gastric juice. It has been studied extensively for its tissue-healing, anti-inflammatory, and musculoskeletal repair properties across multiple organ systems.
02
How does it work?
Cellular Signaling & Healing Cascade
BPC-157 activates angiogenesis (new blood vessel formation), upregulates growth hormone receptors in tendons and muscles, modulates the nitric oxide system to reduce inflammation, stimulates fibroblast activity for collagen production, and downregulates pro-inflammatory cytokines (TNF-α, IL-6).
03
How it helps?
TMJ & Myofascial Benefits
For TMJ patients, BPC-157 accelerates healing of overloaded masticatory muscles, reduces capsular inflammation, supports collagen remodeling in the articular disc and periodontal ligament, modulates chronic trigger point pain, and speeds recovery following dental procedures and orthotic adjustments.
04
What to expect?
Timeline & Protocol
Subjective improvement in pain and muscle tension is often noticed within 2–4 weeks. Full tissue-level changes, including collagen remodeling and disc support, develop over 6–12 weeks. Your protocol will be designed to your case, with follow-up appointments to monitor response and adjust dosing.
Peptide Deep Dive
A Closer Look at Every Peptide We Use
Select any peptide below to explore its mechanism of action, oral health applications, and what patients can expect from treatment.

Enamel Regeneration
Amelogenin-Derived Peptides
P11-4 · Emdogain (EMD) · LRAP
What is it?
Biomineralization Signal Peptides
Amelogenin-derived peptides are short sequences derived from the enamel matrix proteins that orchestrate tooth development. P11-4 (commercially available as Curodont Repair) is a self-assembling peptide that creates a scaffold mimicking the enamel matrix, directing calcium and phosphate ions to rebuild hydroxyapatite crystal structure from within a lesion.
How does it work?
Guided Crystalline Regeneration
When applied to an early carious lesion, P11-4 diffuses into the subsurface demineralized zone and self-assembles into a fibrous matrix. This matrix acts as a nucleation scaffold, attracting and organizing calcium and phosphate ions from saliva into new hydroxyapatite crystals — effectively rebuilding enamel from the inside out without drilling or restoration.
How it helps?
Non-Invasive Caries Reversal
Clinical trials demonstrate that P11-4 can arrest and reverse early-stage (ICDAS 1–2) enamel caries without any tooth preparation. Emdogain (EMD) serves a different but related role in periodontal surgery — it re-creates the enamel matrix environment on root surfaces to regenerate lost periodontal attachment, new cementum, and alveolar bone.
What to expect?
Timeline & Application
P11-4 is applied in a single in-office visit. Radiographic evidence of remineralization typically becomes apparent within 3–6 months. The lesion is monitored at recall appointments. Emdogain is applied during periodontal regenerative surgery and works progressively over 6–12 months as new attachment forms.

Muscle Repair & TMJ
BPC-157
Body Protection Compound · 15-Amino Acid Peptide
What is it?
Gastric-Derived Tissue Healing Peptide
BPC-157 is a stable, synthetic 15-amino acid peptide derived from a naturally occurring protein found in human gastric juice. It has been studied extensively in both animal models and early human trials for its ability to accelerate healing across muscle, tendon, ligament, bone, and neural tissue — with a consistently favorable safety profile.
How does it work?
Angiogenesis, NO Modulation & Cytokine Control
BPC-157 activates angiogenesis to restore blood supply to damaged tissue, upregulates growth hormone receptors in tendons and muscles, modulates the nitric oxide system to reduce localized inflammation, stimulates fibroblast proliferation for collagen synthesis, and downregulates TNF-α and IL-6 — the primary cytokines driving chronic myofascial pain.
How it helps?
TMJ, Masseter & Disc Repair
For TMJ patients, BPC-157 accelerates healing of overloaded masticatory muscles (masseter, pterygoids, temporalis), reduces inflammatory activity within the joint capsule, supports collagen remodeling in the articular disc and periodontal ligament, and modulates the chronic trigger point pain patterns that drive referred jaw headaches. It also speeds post-procedural recovery.
What to expect?
2–12 Week Protocol
Subjective improvement in pain levels and muscle tension typically begins within 2–4 weeks. Structural tissue-level changes develop over 6–12 weeks. Available as subcutaneous injection, sublingual spray, or oral capsule. Your provider will select the delivery method and dose based on acuity of presentation and patient preference.

Collagen & Periodontal Health
GHK-Cu
Glycyl-L-Histidyl-L-Lysine Copper Tripeptide
What is it?
Naturally Occurring Copper-Binding Tripeptide
GHK-Cu is a tripeptide (glycine–histidine–lysine) complexed with copper (Cu²⁺) that occurs naturally in human plasma, saliva, and urine. Plasma concentrations decline significantly with age — from ~200 ng/mL at age 20 to ~80 ng/mL by age 60 — making it a compelling target for age-related tissue maintenance and periodontal health.
How does it work?
Collagen Gene Activation & MMP Inhibition
GHK-Cu activates genes encoding collagen I, III, and elastin production while simultaneously downregulating matrix metalloproteinases (MMPs) — the enzymes responsible for degrading periodontal ligament fibers in periodontitis. It also has potent antioxidant and anti-inflammatory effects, reducing oxidative stress in gingival tissue.
How it helps?
PDL Health & TMJ Disc Support
In periodontology, GHK-Cu supports the maintenance and regeneration of the periodontal ligament — the connective tissue that anchors teeth to the alveolar bone. In the TMJ context, it promotes collagen remodeling of the articular disc and joint capsule, slowing age- and function-related degenerative changes. It also supports wound healing following periodontal surgery.
What to expect?
6–12 Week Tissue Remodeling Window
GHK-Cu works progressively as a tissue remodeling agent. Meaningful collagen-level changes develop over 6–12 weeks of consistent use. It is available as a subcutaneous injection or topical preparation, and is often combined with BPC-157 or Thymosin Beta-4 in multi-peptide TMJ protocols.

Anti-Inflammation & Wound Healing
Thymosin Beta-4
TB-500 · Tβ4 · 43-Amino Acid Peptide
What is it?
Ubiquitous Tissue Repair Peptide
Thymosin Beta-4 (Tβ4) is a naturally occurring 43-amino acid peptide found in virtually every tissue and cell in the body. It is one of the most abundant intracellular peptides in mammals and plays a central role in cell migration, angiogenesis, and tissue protection. TB-500 is the synthetic version used therapeutically.
How does it work?
Actin Sequestration & Cell Migration
Tβ4 works by sequestering actin monomers (G-actin), which regulates cell motility and enables rapid wound closure. It promotes new blood vessel formation, stimulates keratinocyte and fibroblast migration into wound sites, and modulates the inflammatory response by reducing local levels of inflammatory cytokines — all critical to healing after oral surgical procedures.
How it helps?
Post-Surgical Healing & Periodontal Support
In dentistry, Thymosin Beta-4 accelerates extraction socket healing, reduces post-surgical inflammation, supports gingival tissue repair, and may mitigate soft tissue breakdown in aggressive periodontitis. For TMJ patients, it reduces inflammatory activity in the joint capsule and supports the resolution of chronic synovitis.
What to expect?
4–8 Week Anti-Inflammatory Protocol
TB-500 is most commonly administered via subcutaneous injection on a twice-weekly schedule for 4–8 weeks. It is often combined with BPC-157 in post-surgical or acute TMJ inflammation protocols for synergistic tissue repair and inflammation control. Results are typically measurable within 3–4 weeks.

Systemic Anti-Inflammation
KPV &Larazotide
Lys-Pro-Val · AT-1001 · Mucosal Integrity Peptides
What is it?
NF-κB Targeting Tripeptide & Barrier Peptide
KPV (Lys-Pro-Val) is a C-terminal tripeptide of α-melanocyte-stimulating hormone with potent, selective anti-inflammatory activity mediated primarily through NF-κB pathway inhibition. Larazotide acetate (AT-1001) is a tight-junction regulating peptide that strengthens epithelial barrier integrity across mucosal surfaces — including the oral epithelium.
How does it work?
NF-κB Inhibition & Tight Junction Restoration
KPV enters cells and directly inhibits the NF-κB transcription factor — the master regulator of inflammatory gene expression. This reduces production of IL-1β, IL-6, TNF-α, and other cytokines driving chronic oral inflammation. Larazotide works complementarily by binding claudin receptors to restore the tight-junction barriers that, when compromised, allow bacterial endotoxins from periodontal pathogens to penetrate systemic circulation.
How it helps?
Mucositis, Periodontitis & Gut-Oral Axis
KPV is particularly relevant for patients with refractory periodontitis, pericoronitis, chemotherapy-induced oral mucositis, or chronic low-grade gingival inflammation unresponsive to conventional scaling. Larazotide's barrier-restoration effect addresses the bidirectional gut-oral microbiome relationship — strengthening the mucosal defense layer that systemic inflammation and periodontal disease progressively erode.
What to expect?
Oral Capsule Protocol · 6–12 Weeks
KPV and Larazotide are among the few peptides designed specifically for oral delivery — their mechanism of action occurs locally in the GI and oral mucosa. Both are taken as capsules. Measurable reduction in gingival inflammation is typically observed within 4–8 weeks when combined with professional periodontal care.

Bone & Tissue Growth
CJC-1295 &Ipamorelin
GHRH Analogue · GH Secretagogue Combination
What is it?
Growth Hormone Releasing Peptide Stack
CJC-1295 is a synthetic analogue of growth hormone releasing hormone (GHRH) that stimulates the pituitary gland to produce and release growth hormone. Ipamorelin is a selective GH secretagogue that mimics ghrelin's GH-releasing action without stimulating cortisol or prolactin. Together they create a synergistic, physiological pulse of GH that closely mirrors natural release patterns.
How does it work?
Pituitary Stimulation & IGF-1 Upregulation
The CJC-1295/Ipamorelin combination restores youthful pulsatile GH secretion, which drives downstream IGF-1 production in the liver. IGF-1 is the primary anabolic mediator — it promotes protein synthesis, collagen production, bone mineralization, and cellular regeneration. It does this without suppressing the body's own feedback axis, making it significantly safer than direct GH administration.
How it helps?
Implant Healing, Bone Density & Collagen
Optimized GH pulsatility supports osseointegration of dental implants by maintaining osteoblast activity and bone matrix quality. It preserves alveolar bone density in patients experiencing age-related bone loss, accelerates bone graft healing timelines, and promotes systemic collagen turnover that benefits periodontal ligament and TMJ disc integrity. Particularly relevant for implant patients over 45.
What to expect?
3–6 Month Systemic Protocol
CJC-1295/Ipamorelin is administered via subcutaneous injection, typically 5 nights per week before sleep (to align with the body's natural nocturnal GH pulse). Benefits accrue gradually over 3–6 months. Patients often notice improvements in sleep quality, recovery, and body composition — alongside the primary dental goals of better osseointegration and bone maintenance.

Sleep & Bruxism
Selank &DSIP
Tuftsin Analogue · Delta Sleep Inducing Peptide
What is it?
Anxiolytic & Sleep Architecture Peptides
Selank is a synthetic heptapeptide analogue of the immunomodulatory tetrapeptide tuftsin, developed in Russia and studied for anxiolytic, nootropic, and neurotrophic effects. DSIP (Delta Sleep Inducing Peptide) is a neuropeptide that promotes slow-wave (delta) sleep architecture. Both address the neurological drivers of nocturnal bruxism — stress physiology and disrupted sleep.
How does it work?
GABAergic Modulation & Serotonin Balance
Selank modulates the GABAergic and serotonergic systems, reduces anxiety without sedation or dependency, and upregulates BDNF — promoting neural resilience. It also inhibits enkephalin-degrading enzymes, extending the calming effect of endogenous opioid peptides. DSIP works by modulating the hypothalamic-pituitary axis to increase the proportion of deep, restorative slow-wave sleep, during which muscle relaxation is greatest.
How it helps?
Bruxism Reduction & Jaw Muscle Relaxation
Nocturnal bruxism is significantly driven by stress-related sympathetic activation and fragmented sleep architecture. By reducing anxiety and improving slow-wave sleep, Selank and DSIP address these root drivers — reducing the intensity and frequency of nocturnal parafunction. This directly reduces the mechanical loading on the TMJ and masticatory muscles that drives long-term joint and tooth wear.
What to expect?
Nasal Spray Protocol · 4–8 Weeks
Selank is most effectively delivered via intranasal spray (1–2 times daily), providing rapid CNS access via the olfactory pathway. DSIP is administered in the evening before sleep, either intranasally or via subcutaneous injection. Many patients report improved sleep quality and reduced morning jaw pain within 2–3 weeks. Used alongside occlusal splint therapy and TMJ functional treatment for maximal benefit.

Oral Microbiome Defense
Antimicrobial Peptides
LL-37 · Histatins · Human Beta-Defensins
What is it?
Innate Immune Defense Peptides
Antimicrobial peptides (AMPs) are short, positively charged peptides produced by epithelial cells and immune cells as first-line defenses against microbial invasion. In the oral cavity, LL-37 (a cathelicidin), histatins (salivary peptides), and human beta-defensins (HBDs) are produced continuously — but their expression is suppressed by chronic inflammation, poor nutrition, and aging, contributing to periodontal disease progression.
How does it work?
Membrane Disruption & Biofilm Inhibition
AMPs work by inserting into and disrupting the lipid membranes of gram-negative bacteria — including the key periodontal pathogens P. gingivalis, T. forsythia, and T. denticola — without the mechanisms of resistance that plague conventional antibiotics. They also inhibit biofilm formation, modulate the inflammatory response, and promote wound healing in gingival tissue, making them multifunctional oral health agents.
How it helps?
Non-Antibiotic Periodontal Management
AMPs represent a promising direction for managing periodontal disease without the collateral damage to the broader microbiome caused by systemic antibiotics. They selectively target pathogenic bacteria while preserving commensal flora. LL-37 in particular also promotes gingival keratinocyte migration and angiogenesis — accelerating the repair of damaged gingival tissue alongside its antimicrobial function.
What to expect?
In-Office & Adjunctive Topical Protocols
AMP therapy in dentistry is primarily delivered topically — as rinses, gels, or locally applied agents during periodontal procedures. Clinical AMP formulations are an emerging area; our team stays current with available preparations and will advise on what is accessible and evidence-supported for your case. Used alongside professional debridement and home care for maximal benefit.
Administration & Access
How Peptides Enter the Body
Peptide delivery method affects bioavailability, onset time, and patient experience. Our team guides each patient to the right modality based on the specific peptide and treatment objective.
01
Oral Capsule
Moderate Bioavailability
Taken by mouth once or twice daily. Acts partially through local GI mucosal pathways and partially via systemic absorption. Best for chronic low-level inflammation management. Most convenient, no technique required.
02
Sublingual Spray
High Bioavailability · Patient Preferred
Absorbed directly through the mucous membranes under the tongue, bypassing first-pass liver metabolism. Faster and more efficient uptake than oral capsules. Administered once or twice daily — a preferred needle-free systemic option.
03
Subcutaneous Injection
Highest Bioavailability
For TMJ patients, BPC-157 accelerates healing of overloaded masticatory muscles, reduces capsular inflammation, supports collagen remodeling in the articular disc and periodontal ligament, modulates chronic trigger point pain, and speeds recovery following dental procedures and orthotic adjustments.
04
Topical / Intraoral
In-Office · Targeted
For dental-specific peptides — P11-4 for enamel remineralization, Emdogain gel in periodontal surgery, AMP rinses for microbiome management — topical delivery places the active peptide precisely at the target tissue. Applied in-office as part of your dental treatment.
05
Nasal Spray
CNS Access · Fast Onset
Intranasal delivery exploits the rich nasal mucosa vascular bed and — for neuro-active peptides like Selank and DSIP — provides direct access to the CNS via the olfactory pathway. Particularly relevant for sleep and anxiety-modulating peptides that benefit bruxism patients.
Why Core Smiles
Peptide Therapy, Done Right
Peptide therapy is a rapidly evolving field that demands clinical precision, patient education, and institutional accountability. Core Smiles brings all three.
Evidence-Based Protocols
Every peptide we recommend is supported by peer-reviewed research. We don't chase trends — we follow the science.
Licensed Compounding Sources
We source exclusively from FDA-regulated compounding pharmacies meeting USP <797> sterility standards.
Integrated with Your Dental Care
Peptide protocols are designed as complements to your core treatment plan — not standalone products.
Transparent & Informed
Complete informed consent, clear pricing, and ongoing provider monitoring throughout your protocol.
Peptides & Human Longevity
The Oral System as a Window to Aging
The oral cavity is increasingly recognized as a direct proxy for systemic biological age. Periodontal disease accelerates cardiovascular risk. Chronic oral inflammation correlates with insulin resistance and neurodegeneration. Peptide science sits at the frontier of longevity medicine — and the mouth is where it begins.

Have Questions?
Understanding Peptide
Therapy Starts Here
Who might consider peptide therapy?
Peptide therapy is most relevant for patients managing TMJ disorder, myofascial pain syndrome, periodontal disease, chronic oral inflammation, or those seeking to optimize healing around dental implants or surgical procedures. It is also appropriate for patients interested in a longevity-focused approach to oral and systemic health.
Are peptides FDA-approved?
Some peptides are FDA-approved for specific indications (e.g., Emdogain for periodontal regeneration). Others are available through FDA-regulated compounding pharmacies as physician-prescribed compounds. We work exclusively with licensed compounding pharmacies that meet USP <797> sterility standards and will discuss regulatory status at your consultation.
What is the typical treatment experience?
Your consultation includes a thorough review of your dental history, systemic health, medications, and goals. From there, we design a protocol specifying peptide(s), delivery method, dosing, and duration. We provide complete written instructions and onboarding, and schedule follow-up appointments to monitor your response. Most patients start on 4–12 week protocols.
How long until I see results?
Timeline varies by peptide and indication. BPC-157 for musculoskeletal healing often shows subjective improvement within 2–4 weeks. Collagen-stimulating peptides like GHK-Cu typically show tissue-level changes over 6–12 weeks. Enamel matrix peptides like P11-4 show radiographic remineralization changes within 3–6 months. We set clear, evidence-based expectations at every consultation.
Does insurance cover peptide therapy?
Most peptide protocols fall outside standard dental or medical insurance coverage, as many are prescribed off-label or as compounded preparations. We provide transparent pricing at consultation. Some dental procedures that peptides are supporting may remain covered under your plan in the usual manner.
Is there anything to keep in mind?
Peptide therapy is an adjunct to — not a replacement for — your primary dental care. Patients with a personal or family history of cancer, those who are pregnant or breastfeeding, or those taking immunosuppressants should discuss individualized risk-benefit considerations with their provider. A complete health history is required before any protocol is initiated.
I have TMJ. Which peptides are most relevant for me?
TMJ patients are among the strongest candidates for peptide therapy adjuncts. BPC-157 addresses muscular and connective tissue repair; GHK-Cu supports articular disc collagen integrity; Selank and DSIP target the stress and sleep pathways driving nocturnal bruxism; TB-500 accelerates resolution of joint capsule inflammation. We often combine 2–3 peptides in a synergistic TMJ protocol alongside our established functional treatment approaches.
Core Smiles · New York City
Precision Dentistry.
Personalized for You.
At Core Smiles, every peptide protocol is centered on you — your biology, your oral health goals, and your long-term wellbeing. From your initial consultation through your final result, we deliver an experience that is seamless, evidence-based, and carefully curated.
